Your chemotherapy treatment
Your chemotherapy treatment
Chemotherapy is one of the most common cancer treatments. It helps to control the disease after it has spread. The standard of drugs, dosage control and premedication enable treatments to be increasingly effective, achieving improved results with fewer side effects.
What is chemotherapy?
It is the use of drugs, with different mechanisms of action, to attack tumour cells.
- These drugs act on the whole body, with a greater effect on those cells that grow and reproduce more rapidly than normal cells.
- They can destroy tumour cells which have spread, or prevent them from spreading (metastasising), to parts of the body far from the original tumour (primary).
How long does chemotherapy treatment last?
Your oncologist will find the treatment regimen which is best suited to you depending on:
- type of cancer
- stage of cancer
- state of health
- aim of treatment.
Generally treatment is given in cycles composed of a determined number of sessions. A cycle is a period of treatment followed by a period of rest.
A rest is required between cycles so that your body can recover after treatment.
Administration time or session length depends on the drug and the premedication time prescribed.
Patient preparation beforehand
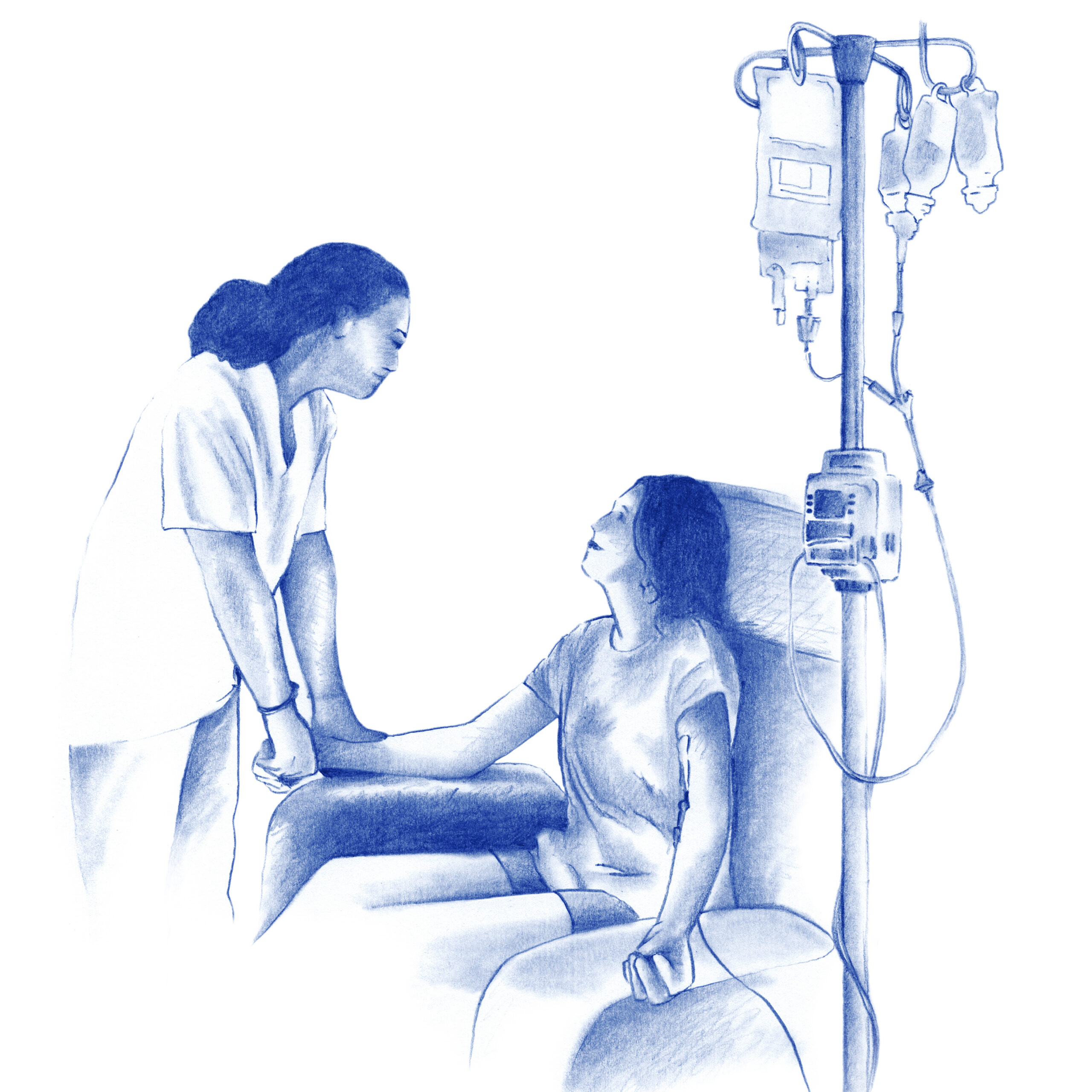
In the majority of cases a specific preparation is not required, however, depending on the type of treatment, your doctor may recommend:
Before treatment:
- Taking premedication beforehand.
- If treatment is long, or uninterrupted, siting of a permanent administration system may be recommended. This could be a reservoir (Porth-a-Cath) or PICC, both are devices with a catheter that directly reaches a large-sized vein.
- Requesting tests and blood analysis, to ensure that your body is prepared for treatment.
- Preparing for side effects such as:
- Hair loss, whether you would like to use a scalp cooling cap (Dignicap®).
- Infertility, whether you might consider egg or sperm preservation for use in the future.
The day of the session
- Your oncologist will assess whether your state of health is appropriate for you to undergo treatment.
- Treatment will be given in the day hospital, by a specialist nurse.
- In the majority of cases patients can drive after treatment, however, it is recommended that you always do so accompanied.
Sometimes treatment may require pre- or post-medication which the nurse will give via the same route, with the aim of minimising side effects
What is the aim of chemotherapy?
Chemotherapy can be given as a single treatment or in combined therapy with other types of treatment such as radiotherapy or surgery, targeted therapy, or hormone therapy.
The intention of treatment may be:
- To eliminate possible remaining tumour cells following surgery (adjuvant).
- • To reduce the tumour or prevent it from spreading (metastasising) before surgery (neoadjuvant).
- • To control disease-related symptoms.
- To enhance another treatment given at the same time (concomitant), generally radiotherapy.
How is chemotherapy given?
Your oncologist will assess the most appropriate administration route for you, it may be:
Intravenous:
medication is given directly into the vein. When treatment is long or has numerous sessions, permanent administrations systems may be recommended as these prevent having a needle inserted at every session and possible complications. We can use these systems to extract blood for analysis and to administer medication. There are two alternatives:
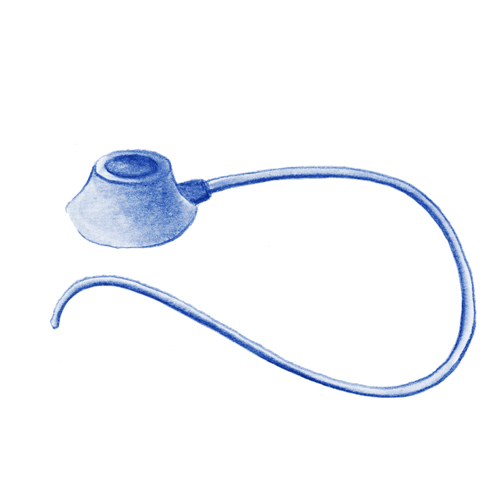
Reservoir (Port-a-Cath®);
- It is roughly the size of a two euro coin.
- It is very comfortable as it is covered by the skin, allowing a normal lifestyle between cycles.
- It includes a catheter which goes through the vein to a large vein close to the heart.
- It allows drugs to be given and blood to be taken.
- It is inserted using minor surgery under local anaesthetic.
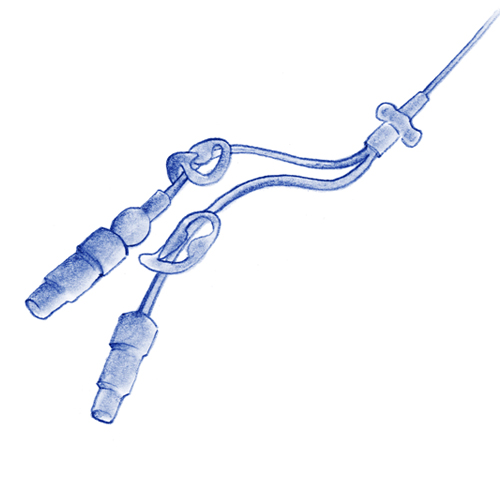
PICC -Peripheral insertion of central catheter.
- It is inserted in a deep vein in the inner arm and is directed towards a major vein near to the heart.
- Insertion is done easily, by a specialist nurse, under ultrasound guidance and as an outpatient.
- The external end must be cared for and should not be blocked.
- It is easy to remove either in the case of complication or at the end of treatment.
Oral:
The drug is dispensed in tablet form. Your oncologist will prescribe treatment and will monitor you to ensure that treatment is tolerated and effective.
Intrathecal:
Given via lumbar puncture, the aim is for the drug to remain in the space surrounding the spinal cord, together with the cerebrospinal fluid. It is more commonly used in haematological cancers.
Intraoperative:
Administered directly to the tumour, during surgery.
Chemotherapy side effects
Side effects depend highly on the drug, dose, and regimen as well as how the chemotherapy is tolerated by the patient. Premedication helps us to control toxicity and reduce side effects.
Possible side effects:
- Digestive abnormalities: nausea, vomiting, diarrhoea, loss of appetite…
- Changes in sense of taste or smell.
- Mouth ulcers
- Fatigue
- Tendency to bruise.
- Advice for dealing with side effects
- Changes in hair, skin and nails: some types of chemotherapy can cause hair loss, this hair loss can have an emotional impact. There are different solutions including hairpieces, extensions, or scalp cooling systems (Dignicap®), the latter directly prevent chemotherapy reaching the scalp to prevent hair loss.
- Effects on fertility: Infertility in the oncological patient depends on:
- The type, stage and site of the tumour.
- The age and sex of the patient.
- Chemotherapy dose and drug.
- In young, fertile patients who wish to have children, egg or sperm preservation may be considered prior to treatment.
- Would you like to know more about preserving fertility?
How do I know if my chemotherapy is working?
Before, during and after treatment, your oncologist will request different tests to check treatment response.
These may be:
- Clinical response: the patient has symptoms of the disease which are reduced or disappear after having treatment.
- radiological response: comparing various radiological investigations with previous ones.
- Biochemical response: monitoring of tumour markers such as PSA during treatment.
- Pathological response: on neoadjuvant treatment. When chemotherapy is administered prior to surgery, the tumour is checked to see how it has responded after surgical removal.
Can I continue with my normal routine during chemotherapy treatment?

You must continue with your normal daily routine and working life whenever possible.
Bear in mind the following recommendations:
- Avoid the sun.
- Maintain nutrition, a Mediterranean diet is recommended. A specialist nutritionist can help you to supplement the necessary nutrients.
- Exercise daily.This is very important, it reduces toxicity, lack of energy, cardiovascular risk… Each individual patient must follow their own personally developed exercise regime.
- Take care of yourself emotionally, a psycho-oncologist will help you to manage the emotional process of the disease.
Other treatments

Inmunotherapy
Boost your immune system. Your own immune cells kill tumor cells.
Targeted therapy
Boost your immune system. Your own immune cells kill tumor cells.
Hormono therapy
Eliminate or decrease the production of hormones. It stops your tumor from growing and spreading.
Would you like more information?
We can contact you, or if you prefer, call us on 952 908 898
Subscribe to our newsletter
HC Marbella you can access information relevant and topical written by different professionals of our medical health units.